AI Case Study: Lessons from an AI project to save £2.3m in Hospital costs
Transforming hospital operations to create AI at scale is more than just tech
Over 15 years, I've taken AI-powered simulations from pilot to enterprise scale across sectors, from car manufacturing and oil & gas to hospital clinical workflows.
In the first of a series, I discuss my experience designing and deploying enterprise AI solutions.
This week’s case study explores a Hospital in the UK, where I was responsible for developing the AI product strategy and delivery of a simulation platform that would model thousands of patient pathways.
My role as product lead centred on translating complex simulation capabilities into operational healthcare value whilst ensuring clinical governance and regulatory compliance.
The pilot delivered impressive efficiency gains across patient flow management. Still, when attempting to scale the AI simulation across the organisation's complex clinical pathways, hidden integration complexities and stakeholder resistance threatened the entire £50M digital transformation investment.
Let’s tuck into the lessons learnt.
The Challenge: When an AI Pilot hits Enterprise Healthcare Reality
Most healthcare organisations treat AI initiatives like traditional IT projects.
They're not.
Enterprise healthcare AI transformations fail in predictable ways:
Through inadequate clinical stakeholder alignment,
Unrealistic integration timelines with legacy systems,
Insufficient governance frameworks for patient safety,
hidden operational costs that weren't factored into the original business case.
For this hospital, looking to implement AI into its operating model, I faced the classic enterprise constraint:
“How do you implement cutting-edge AI within existing clinical workflows, regulatory compliance requirements, and budget limitations, whilst maintaining patient safety standards that legacy systems simply cannot support?”
The enterprise healthcare reality I had to navigate was complex.
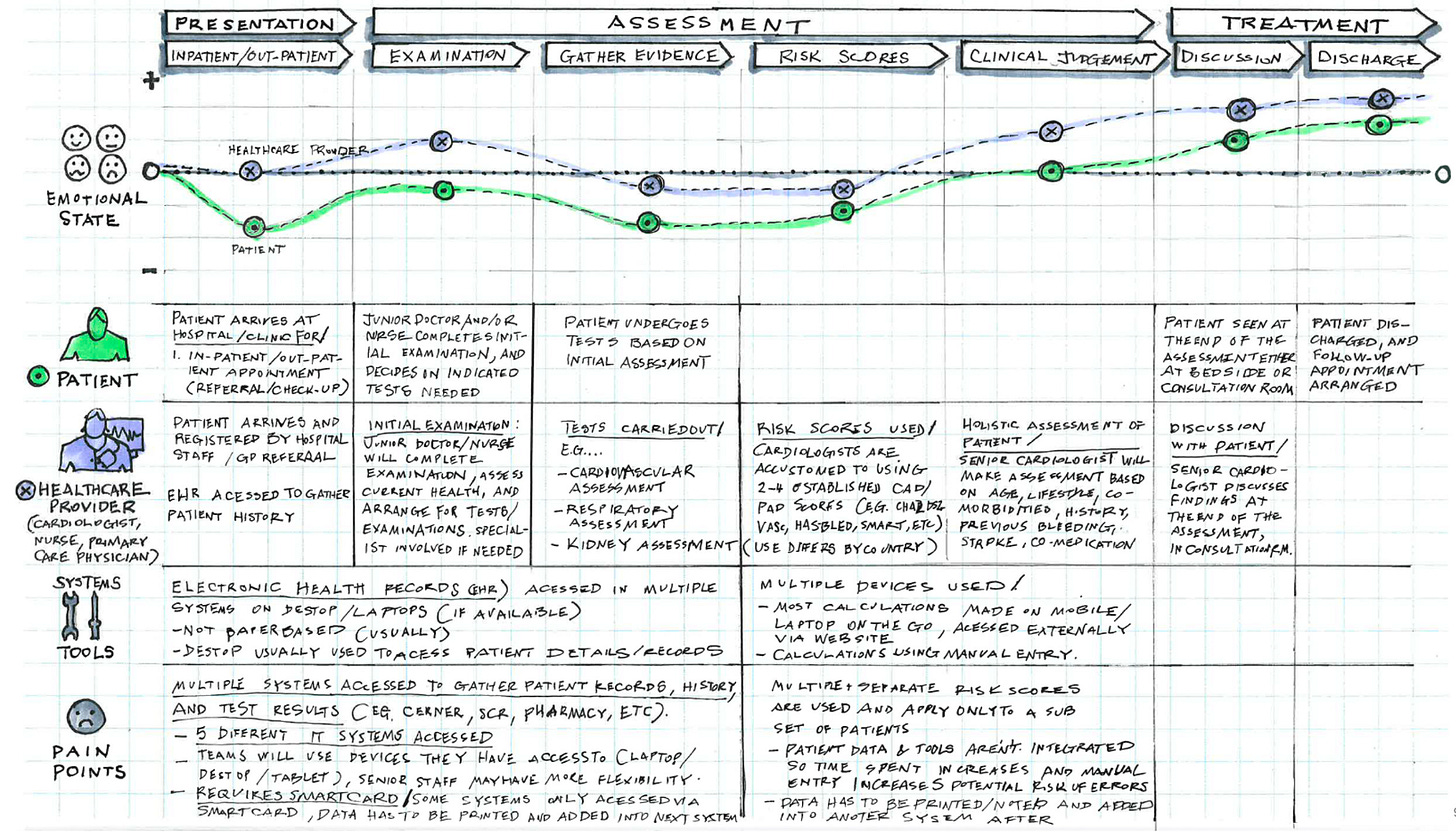
Legacy EHR integration meant we couldn't simply ‘deploy an AI solution’. It required methodical integration with existing clinical information systems that had evolved over decades.
Clinical governance required us to operate within Hospital frameworks and patient safety protocols that weren't designed for AI decision-making.
The stakeholder complexity was immense, requiring buy-in from clinical teams, IT security, medical directors, and hospital executives, each with different priorities and concerns.
European Regulatory Compliance added another layer of complexity.
My team of 35 had to navigate GDPR requirements and UK Government Digital Standards for public sector compliance, whilst proving clinical efficacy in an environment where patient safety cannot be compromised for innovation.
The most challenging part, though?
Maintaining operational continuity. The hospital could not stop operating during transformation, requiring us to balance innovation pressure with the reality that any system failure could directly impact patient care.
The Solution: A Systematic Enterprise AI Simulation Framework
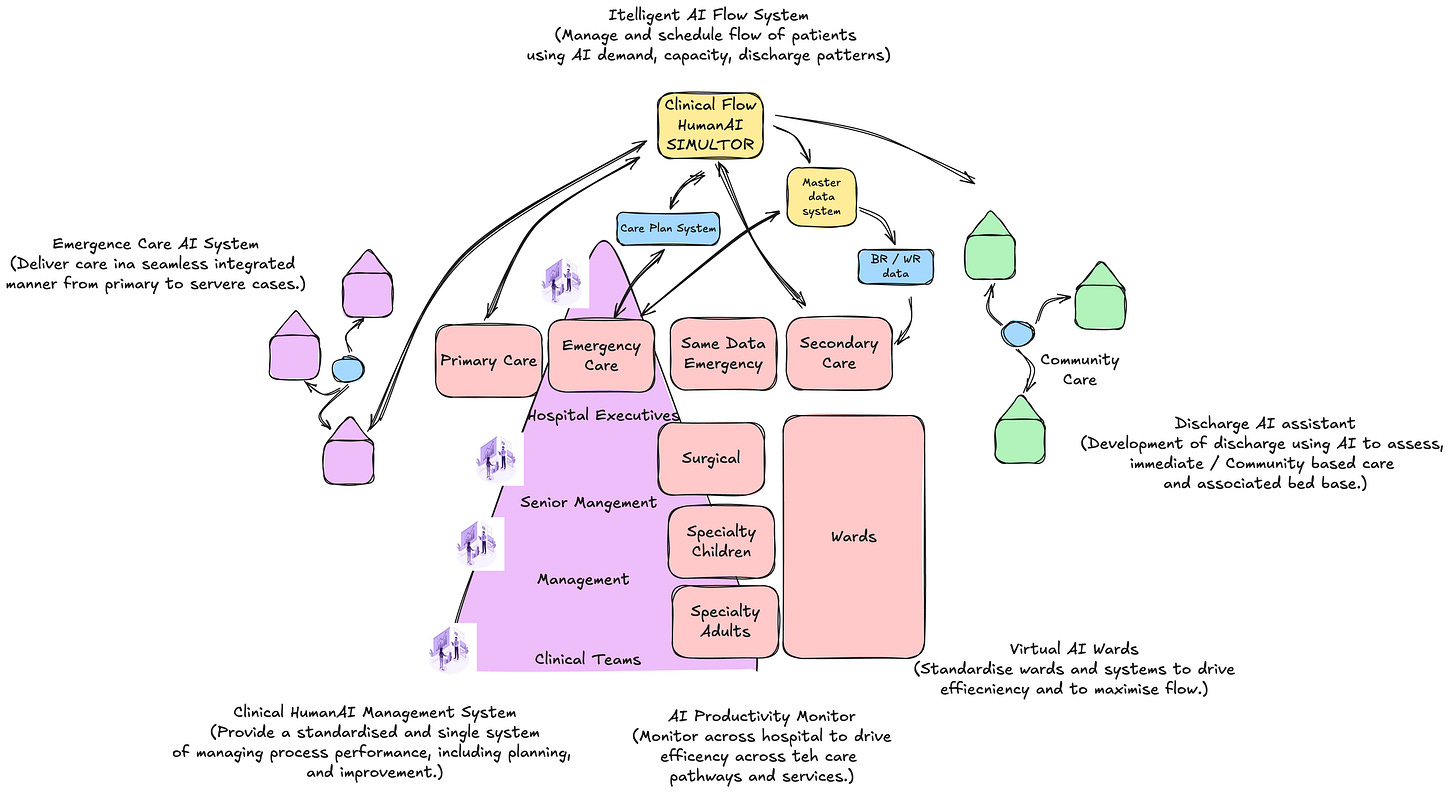
Rather than deploying another point solution, I collaborated with the team to implement a portfolio of products already in use across logistics in car manufacturing. The result was a comprehensive Digital Control Simulator.
This hospital-wide simulation platform addressed the fundamental constraints facing AI transformation.
This wasn't just another technology deployment; it was a complete reimagination of how a hospital could use AI to transform operations whilst working within existing constraints.
The Three-Pillar AI Implementation Strategy
Pillar 1: Clinical-First Design Methodology
Drawing from my cross-sector experience, I insisted on working directly with clinical teams from day one.
“Too many AI projects fail because they're designed by technologists who don't understand the nuances of clinical workflows.”
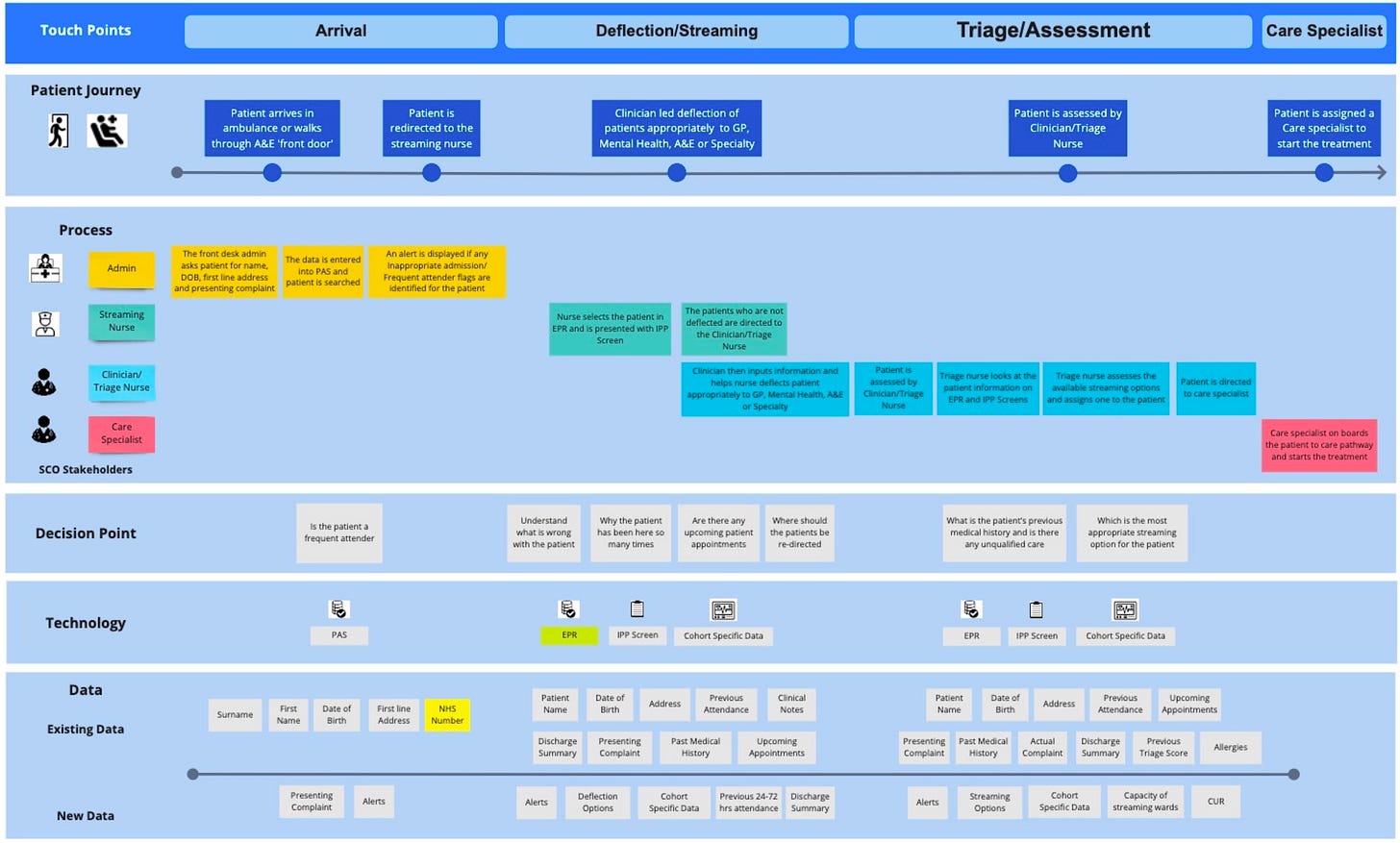
The approach mapped existing patient pathways before building any technology, avoiding the classic mistake of retrofitting AI onto incompatible workflows.
Facilitating weekly design sessions with nurses, doctors, and operational staff, treating them as co-designers rather than end users. This collaborative approach revealed insights that pure data analysis would have missed.
For instance, the clinical teams identified critical handoff points between departments where AI could provide the most value, and they helped us understand the informal protocols that weren't captured in official documentation but were essential for patient safety.
The workflow mapping process involved patient data stories and journeys analysis from admission to discharge. Still, more importantly, it captured the decision-making processes that clinical staff used at each stage.
This understanding became crucial when designing AI recommendations that clinicians would actually trust and use.
Pillar 2: Simulation-Native Architecture
Instead of traditional digital twins requiring massive infrastructure investment, we designed lightweight simulation capabilities that could integrate with existing systems.
The architecture used frameworks enriched with clinical knowledge, combined with live hospital data from EHRs and geometric inputs from IoT sensors tracking patients, staff, and equipment.
This approach was revolutionary because it eliminated the need for the hospital to replace existing systems, a requirement that kills most digital transformation projects before they start.
Two key learnings from replacing existing systems:
Focusing on real-time data integration through direct feeds from existing hospital systems,
Create a simulation layer that models scenarios without disrupting current operations.
Scenario modelling capabilities allowed the hospital to test operational changes before implementation, essentially providing a ‘rehearsal’ environment for any significant operational decision.
This capability alone transformed how the hospital approached change management, moving from intuition-based decisions to evidence-based planning supported by simulation results.
Pillar 3: Governance-Embedded Delivery
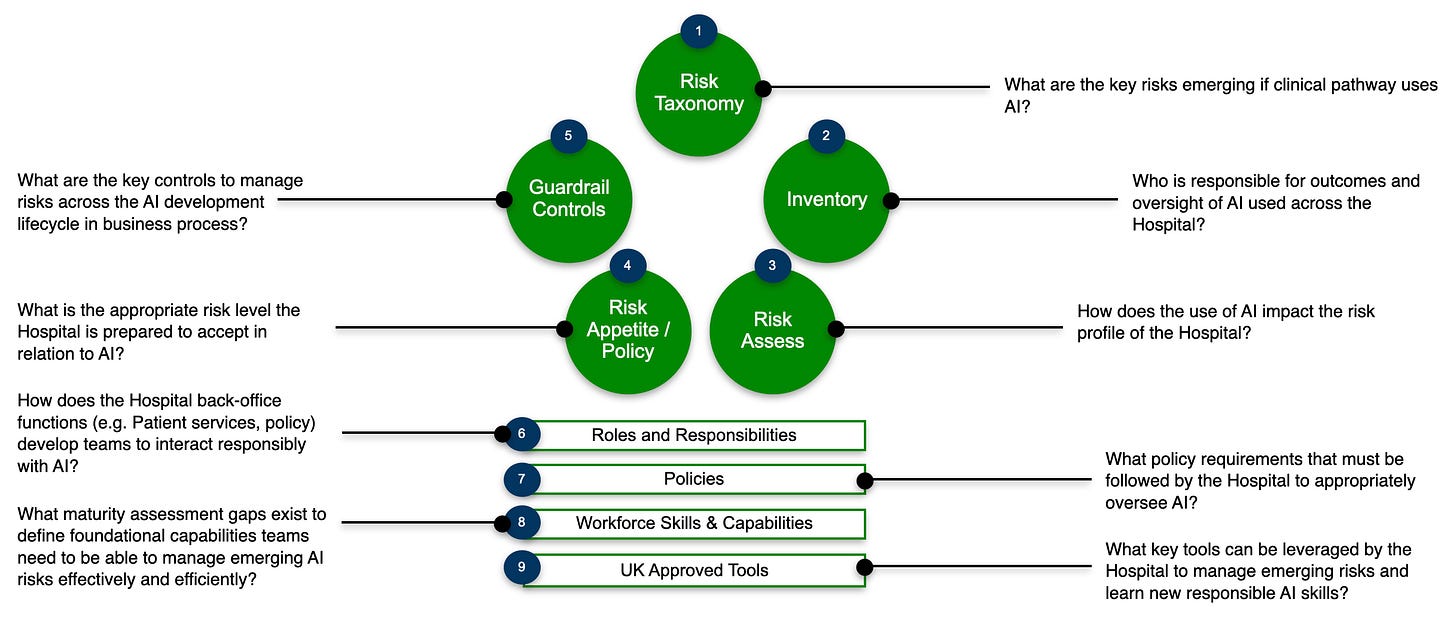
From my experience with complex enterprise transformations, governance cannot be an afterthought.
For this hospital, a clinical governance and risk management framework was needed in every sprint, ensuring regulatory compliance whilst maintaining innovation velocity.
This approach was counterintuitive to many in the technology team who saw governance as a barrier to progress.
“My experience has taught me that early governance integration actually accelerates deployment by removing approval bottlenecks.”
The governance framework was designed to ensure that AI recommendations always included confidence levels and clinical justification, making the decision-making process transparent to clinical staff.
Change management was embedded throughout the implementation rather than treated as a separate workstream. Working with clinical staff to understand their AI concerns helped to design training programmes that built confidence with the technology whilst respecting their clinical expertise.
Business Impact: What the Strategy Delivered to Demonstrate Healthcare Outcomes
The financial returns from this AI strategy demonstrated the sustainable value of simulation-native healthcare operations.
The Approach Delivered:
£2.3M annual cost savings through AI-optimised patient flow,
92% patient visibility across the entire hospital.
2-day improvement in bed utilisation across multiple wards
The transformation became genuinely self-funding, with each use case designed to deliver measurable ROI that justified continued investment. This financial discipline was crucial for sustaining executive support throughout the inevitable challenges of enterprise transformation, and it provided a model that other Hospitals could follow with confidence.
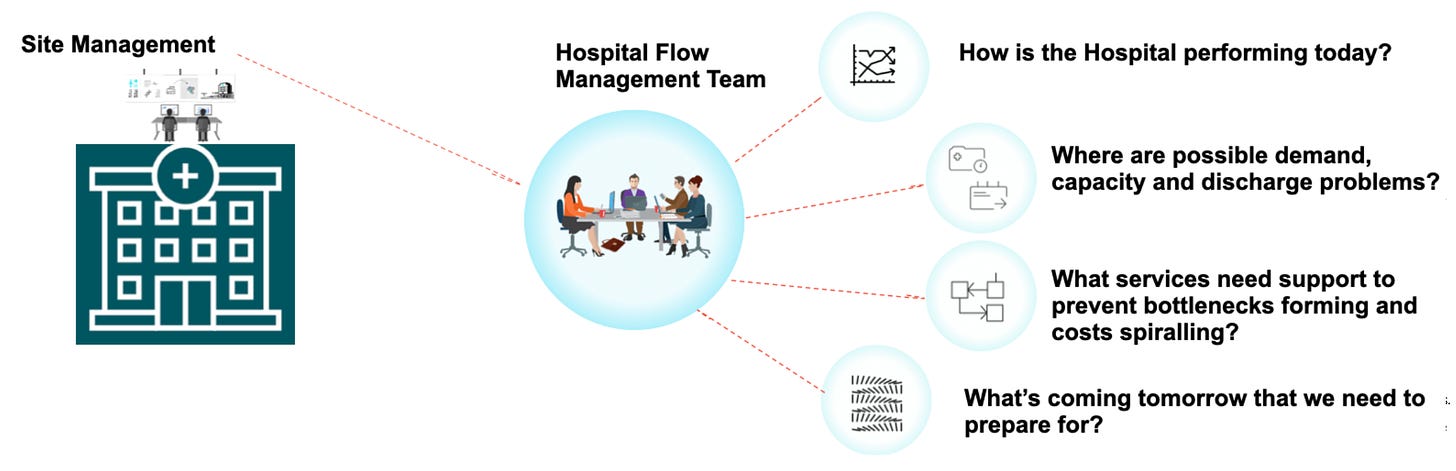
Operational excellence emerged through the simulation framework, delivering improvements that surprised even optimistic projections. The 92% patient visibility came from monitoring patient flow, which used real-time data to anticipate problems before they became critical.
Perhaps most significantly, we achieved a 2-day improvement in bed utilisation across multiple clinical areas using capacity planning algorithms developed that could predict demand patterns and optimise resource allocation in real-time.
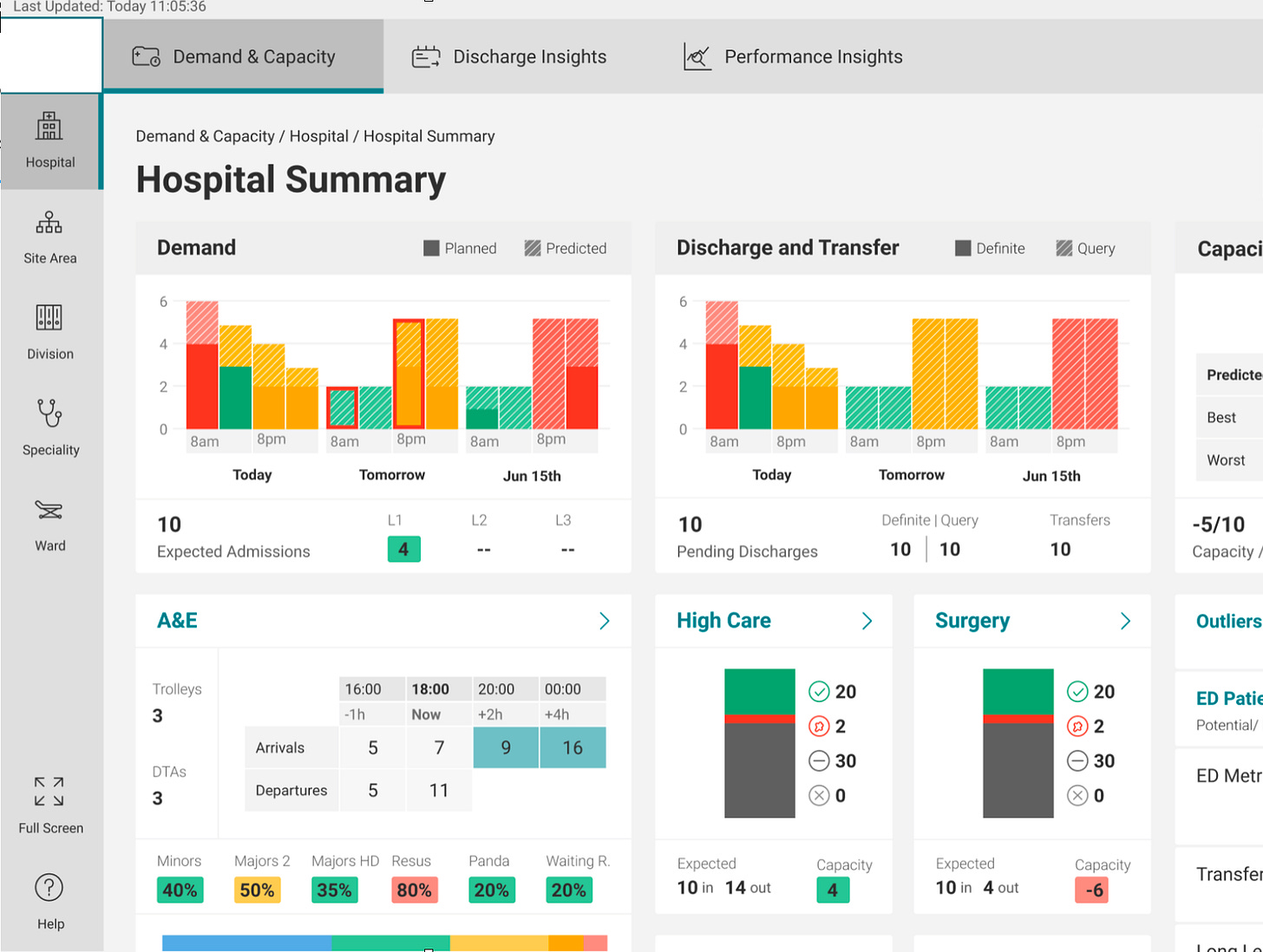
Enhanced patient flow visibility enabled proactive capacity management through real-time dashboards. These were specifically designed for clinical workflows.
Predictive alerts for potential clinical deterioration used early warning algorithms that learned from historical patterns whilst respecting the complexity of individual patient presentations.
The real-time AI simulation enabled the optimisation of staffing models that improved both staff satisfaction and patient outcomes. Reduced patient waiting times resulted from intelligent resource allocation systems that could anticipate bottlenecks and automatically suggest interventions to maintain flow.
Key Strategic Learnings from My Implementation
There are several key learnings when implementing an AI solution in healthcare settings:
1. Clinical Engagement Is Non-Negotiable
The most sophisticated AI simulation platform fails without clinical champion involvement from project inception. The success of this project stemmed from treating clinical staff as co-designers, not end users, a principle I'd learned from manufacturing transformations.
2. Simulation Before Implementation
Every operational change must be tested in a simulation environment before clinical deployment. This approach eliminates the traditional risk of failed pilots damaging credibility for years.
3. Integration Architecture Determines Success
Rather than replacing existing systems, the winning approach is integrating AI capabilities into current clinical workflows. This reduces implementation risk whilst maximising adoption.
4. Governance Enables Innovation
Embedding clinical governance and safety protocols from day one accelerates deployment by removing approval bottlenecks that typically delay healthcare AI projects, a lesson from my previous enterprise transformations when regulation is involved.
5. Financial Discipline Drives Sustainability
Each AI use case developed included specific ROI calculations and measurable business outcomes. This financial rigour enables continued investment and scaling across a healthcare setting.
The Broader Healthcare AI Opportunity
This case study documents an approach to enterprise healthcare AI transformation, proven successful across multiple complex operational environments.
The methodologies developed provided a systematic framework for AI implementation within healthcare governance constraints whilst delivering measurable business impact.
I welcome conversations with anyone leading similar transformation initiatives. My simulation-native approach offers significant opportunities for hospitals seeking measurable AI impact whilst maintaining clinical safety and regulatory compliance.